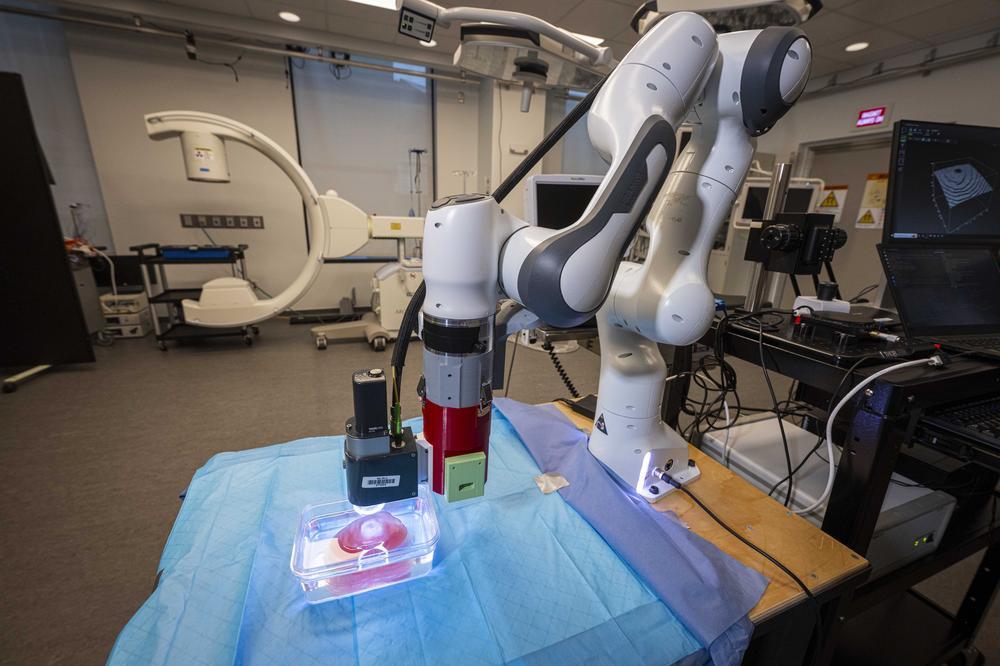
A novel robotic system that can operate inside the bore of an MRI scanner is currently being tested as part of a biomedical research partnership program at Brigham and Women’s Hospital in Boston with the aim of determining if the robot, in conjunction with real-time MRI images, can make prostate cancer biopsies faster, more accurate, less costly, and less discomforting for the patient. The novel system also has the potential to deliver prostate cancer therapies with greater precision.
Developed by a team of robotics engineers at Worcester Polytechnic Institute (WPI) in collaboration with colleagues at Johns Hopkins University, Brigham and Women’s Hospital (BWH) and Acoustic MedSystems Inc., the robotic system is being used in the BWH Advanced Multimodality Image-Guided Operating suite (AMIGO).
"Prostate cancer is the last form of cancer still diagnosed with blind needle biopsies, so we are working to change that with image-guided technology," said Clare M. Tempany, MD, professor of radiology at Harvard Medical School, chair of research radiology at Brigham and Women’s Hospital, and principal investigator for the research program. "The ultimate goal of our group is to develop enabling technologies that extend the capabilities of physicians to treat their patients."

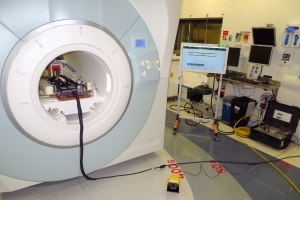
The "first-in-human" testing of the robotic system is also the culmination of more than six years of research and development by Gregory Fischer, associate professor of mechanical engineering and robotics engineering at WPI and director of WPI’s Automation and Interventional Medicine (AIM) Robotics Research Laboratory. Fischer has pioneered, along with Iulian Iordachita and colleagues from the Laboratory for Computational Sensing and Robotics (LCSR) at the Johns Hopkins University, the development of compact, high-precision surgical robots that are expressly designed to work in the environment inside the bore of an MRI scanner, as well as the electronic control systems and software needed to operate the robots with the safety, reliability, and ease of use required of technology designed for the operating room.
"The robot gives the physician a great deal more choice about where to place the biopsy needle," Fischer said. "This technology should permit greater accuracy, and the odds of hitting the target on the first try should be higher. The anticipated result is fewer needle placements with higher sensitivity, a faster procedure, less need for repeated biopsies, lower overall cost, and reduced discomfort for the patient."
Currently in the United States, most prostate biopsies are performed in conjunction with ultrasound imaging. While an ultrasound scan can localize the prostate, the imaging modality cannot determine where the potential cancer may be. Therefore, the biopsies are conducted randomly with repeated needle insertions seeking to remove samples from the cancerous tissue. These procedures suffer from low sensitivity and may produce misleading results. In fact, about 35 percent of serious tumors may be missed during initial biopsies that are guided solely by ultrasound. Because of the high error rate, patients frequently need to return for repeated biopsies as their symptoms persist and their tumors continue to grow.
MRI, on the other hand, can produce detailed anatomical and tissue-characterization images of the prostate and detect potentially cancerous lesions. For that reason, there is significant interest nationally in developing methods for using real-time imagery from MRI alone or in conjunction with ultrasound to guide the insertion of needles for prostate biopsies. Eventually, if the robotic technology proves effective, it could easily be adapted to deliver therapies directly to the tumors within the prostate, Dr. Tempany noted.
In biopsies now conducted as part of a Brigham and Women’s program without the new robot, physicians use a plastic grid to help position the biopsy needle. They first use multi-modality MRI scans to generate a plan showing where the needle should be inserted, then with the patient in the MRI scanner, the physician directs the needle through most appropriate guide holes in the grid. Additional scans are made periodically to verify the path of the needle and make adjustments, if needed.
Rather than restrict the needle positioning to the choices offered by the grid, WPI/JHU ’s MRI-compatible robot manipulates a needle-guide inside the bore of the scanner to help the physician place the needle in the most optimal position as indicated by the real-time images generated by the MRI.
To develop robots that can work inside an MRI scanner, Fischer and his team have had to overcome several significant technical challenges. Most important, since the scanner includes a powerful magnet, the robot, including all of its sensors and actuators, must be made from non-ferrous materials. The robot used in the prostate cancer trial is built primarily of plastic parts and uses ceramic piezoelectric motors. In addition, a low-noise WPI-developed custom control system and well-shielded wiring help to prevent the emission of electrical signals that could mar the MRI images. The robot must also be small enough to fit in the cramped confines of the MRI bore and still leave room for the patient and the clinician’s hands. "On top of all this, we had to develop the communications protocols and software interfaces for controlling the robot, and interface those with higher-level imaging and planning systems," Fischer said. "That added up to a massive systems integration project."
Creating a system that can be used in clinical practice added another layer of complexity, Fischer said. To begin with, the robot must be easy for a non-technical surgical team to sterilize, set up, and place in the scanner. "It needs to be easy to use and foolproof," he said. "It required many iterations of the hardware and software to get to that point."
In addition, the system includes highly enforced workflows to ensure that procedures are carried out in the correct order and the same way each time the system is used. The system also has robust error detection to alert the staff should a cable become unplugged or other unexpected problems occur. "We wanted to be sure that an error will cause the robot to safely stop," Fischer said, "but we also wanted to the system to be able to recover and continue, if possible, without having to start the procedure all over again. We spent a great deal of time on risk mitigation, figuring out all of the ways the system could fail and what we would do in each and every case."
The test of the robot system is an important component of a larger clinical research program at Brigham and Women’s Hospital funded by a Bioengineering Research Partnership award from the National Institutes of Health through the National Cancer Institute.* Under way since 2006, the program has received more than $7 million in NIH support for development of an FDA-approved image-guided platform for use with MRI or ultrasound, which can aid in baseline imaging, diagnostic biopsy, and treatment of prostate cancer.
In Fischer’s AIM lab (aimlab.wpi.edu), work is also under way on a next-generation robotic system that, in addition to positioning a needle guide, will also robotically actuate the insertion and help steer the needle to a target of interest. "We hope to be able to test that system with patients in a year or so," Fischer says. "We are also looking forward to collaborating with Brigham and Women’s Hospital and other partners to test the use of our system not just in prostate cancer diagnosis, but to deliver therapy, whether brachytherapy or ablation therapy."
WPI’s modular MRI-compatible robotic system can be readily adapted for other surgical applications. For example, Fischer is the principal investigator on a $3 million R01 award from the National Cancer Institute, through which he and a team that includes colleagues at Albany Medical College, the University of Massachusetts Medical School, and Acoustic MedSystems are developing a robotic system that, guided by real-time MRI imagery, will insert a probe though a dime-sized opening in the cranium to destroy brain tumors using interstitial high-intensity focused ultrasound.
* "Enabling Technologies for MRI-Guided Prostate Interventions," NIH project No. R01CA111288-09
About Brigham and Women’s Hospital
Brigham and Women’s Hospital (BWH) is a 793-bed nonprofit teaching affiliate of Harvard Medical School and a founding member of Partners HealthCare. BWH has more than 3.5 million annual patient visits, is the largest birthing center in Massachusetts, and employs nearly 15,000 people. The Brigham’s medical preeminence dates back to 1832, and today that rich history in clinical care is coupled with its national leadership in patient care, quality improvement and patient safety initiatives, and its dedication to research, innovation, community engagement and educating and training the next generation of health care professionals. Through investigation and discovery conducted at its Brigham Research Institute (BRI), BWH is an international leader in basic, clinical and translational research on human diseases, more than 1,000 physician-investigators and renowned biomedical scientists and faculty supported by nearly $650 million in funding. For the last 25 years, BWH ranked second in research funding from the National Institutes of Health (NIH) among independent hospitals. BWH continually pushes the boundaries of medicine, including building on its legacy in transplantation by performing a partial face transplant in 2009 and the nation’s first full face transplant in 2011. BWH is also home to major landmark epidemiologic population studies, including the Nurses’ and Physicians’ Health Studies and the Women’s Health Initiative.